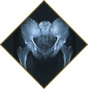
Transient Osteoporosis of the Hip
Transient osteoporosis of the hip is a rare condition that causes bone loss temporarily in the upper part of the thighbone (femur). It is mostly found in young or middle aged men between the ages of 30 and 60, and women in their later stages of pregnancy or early postpartum period (following childbirth). It is characterized by abrupt onset of pain that increases with activity.
The hip joint is a ball-and-socket joint. A part of the pelvis bone known as the acetabulum forms the socket and the upper end of the femur, known as the femoral
head, forms the ball. In patients with transient osteoporosis of the hip, the femoral head loses its density and strength and becomes more prone to breaking.
Causes
An exact cause is unknown. Some of the proposed causes include atypical mechanical stresses acting on the hip joint, hormonal abnormalities, and blockage of some of the small blood vessels surrounding the hip joint.
Symptoms
Symptoms may include
- Unknown pain in the hip not triggered by any previous accident or injury
- Abrupt onset of pain in the anterior thigh, the side of the hip, groin, or buttocks
- Pain that increases with activities or weight bearing and decreases with rest
- Intense pain with extreme hip range of motion
- Gradually increasing pain that becomes disabling over a few weeks or months
- A prominent limp
Diagnosis
Diagnosis of transient osteoporosis of the hip often begins with a history and physical examination. Your doctor may ask you questions related to your general health and any previous accidents or injuries. You will be asked to perform various range-of-motion exercises in order to replicate your pain. Most patients experience acute pain with weight bearing and active range of motion and minimal pain when the doctor moves the hip for them (passive range of motion). This is one of the indicators in the diagnosis of transient osteoporosis of the hip.
You will also be recommended to undergo imaging studies such as X-rays, CT scans, MRIs, or nuclear scans in order to further document transient osteoporosis of your hip.
Most patients with transient osteoporosis of the hip are found to have bone marrow oedema. Bone marrow oedema is a condition where fluid builds up in the bone marrow (spongy material located in the hollow of the long bones) and the bone marrow becomes inflamed. MRI scans have been found to be particularly beneficial in
documenting bone marrow oedema and are one of the most practicable studies in the diagnosis of transient osteoporosis of the hip.
Treatment
Transient osteoporosis of the hip resolves on its own and treatment involves preventing any damage to the weakened bones and minimizing the symptoms and discomfort. Treatment includes
- Medication: Non-steroidal anti-inflammatory medications or NSAIDs may be recommended to alleviate inflammation and pain
- Restricted weight bearing: You may be recommended to restrict or to completely avoid putting weight on your hip joint. You may need to use walking aids such as crutches, cane, or a walker in order to limit the stresses on your hip bone.
- Physical Therapy: Your doctor may instruct you on special exercises to help strengthen the muscles supporting your hip. Water exercises have been found to be helpful as they ease movement and also relieve weight bearing.
- Nutrition: Vitamin D and calcium have been found to be effective in healing and rebuilding of bones. Your doctor will recommend you foods or supplement that can help you recover faster.
Incision care
Some of the instructions that you will be given with regard to incision care include:
- Keep the incision dry and covered with a light dressing until the staples are removed.
- Inform the physician if there is increased redness, drainage, odour or pain around the incision.
- Inform the surgeon immediately if the patient’s temperature rises above 100.5°F.
Controlling pain and discomfort
Caring for the patient will include various methods of helping the patient control post-surgical pain.
- Pain medications should be given at least 30 minutes before physical therapy.
- You can encourage the patient to gradually reduce pain medications.
- Use ice for about 20 minutes every hour to control pain.
- Encourage the patient to change position every 45 minutes.
Recognizing and preventing complications